Modeling Pathways to Describe How Maternal Health Care Providers' Mental Health Influences the Provision of Respectful Maternity Care in Malawi
Population Council (Burnett-Zieman, Warren); Kamuzu University of Health Sciences (Chiundira, Mandala, Mboma, Kamanga, Kazembe); Ministry of Health, Lilongwe, Malawi (Kachale, Mchoma)
"Without identifying and addressing burnout among maternal health (MH) providers, efforts to achieve respectful maternity care (RMC) will not be reached."
Poor maternal health (MH) provider attitude is often cited as a reason why women may not seek care or delay seeking care at facilities. MH providers may at times fail to provide respectful maternity care (RMC), leading to poor birth outcomes. Traumatic events, such as maternal or fetal death, poor working relationships, and under-resourced environments not only affect providers' own emotional well-being but also reduce their ability to provide RMC. This article seeks to expand the literature on factors related to MH provider burnout and self-reported RMC to improve understanding of barriers to providing quality obstetric care. It is part of a larger implementation research portfolio supported by the United States Agency for International Development (USAID) through the Advancing Postpartum Hemorrhage Care partnership in Malawi.
Data were collected in mid-2021 as a cross-sectional survey with 302 MH providers working in 25 maternities in 3 districts in Malawi. MH providers interviewed were nurse-midwife technicians (59%), registered nurses or midwives (24%), physicians or clinicians (10%), and community midwife assistants (7%). The researchers used: the provider-reported person-centred maternity care scale to measure RMC; the Maslach Burnout Inventory, which examines emotional exhaustion, depersonalisation, and professional accomplishment, to measure burnout; and standard validated screening tools to measure the prevalence of depression and post-traumatic stress disorder (PTSD).
Although levels of burnout varied, 30% of MH providers reported high levels of exhaustion, feelings of cynicism manifesting as depersonalisation toward their clients (17%), and low levels of professional accomplishment (42%). Moderate to severe depression (9%) and suicidal ideation within the past 2 weeks (10%) were also recorded. Many (70%) reported experiencing an event that could trigger PTSD, and 12% reported at least 4 of 5 symptoms in the PTSD scale.
The paper presents a pathway model describing how these factors interact and influence RMC. Path analysis suggests that depression and emotional exhaustion negatively influence RMC, and depersonalisation is mediated through depression. PTSD has no direct effect on RMC, but increased PTSD scores were associated with increased burnout and depression scores.
Despite the detrimental effects of increased levels of PTSD, depersonalisation, emotional exhaustion, and depression on RMC, the study finds that an MH provider's relationship with the facility management (e.g., how they involve MH providers in decision-making processes) can have a powerfully protective effect in this situation. Elsewhere, it has been found that where providers have agency to make decisions, work as a team to share workload, and have a supportive management structure, they were able to overcome structural deficiencies (inadequate equipment, supplies, and space) to provide quality care. Thus: "Pragmatic approaches for improving teamwork, psychosocial, and managerial support for MH providers working in challenging environments may go a long way to mitigate burnout, improve MH provider well-being and, in turn, improve RMC for all women seeking MH care."
Reflecting on existing and potential future studies, the researchers note that, "While it is not surprising to find that MH provider mental health influences RMC provision, there are limited studies demonstrating a clear pathway in a low-income country like Malawi....[F]urther research is needed to improve generalizability and further develop this model of provider mental health..." They point to "the need to understand the situation from the health workers' viewpoints to inform policy and practice. Indeed, the idea for this analysis originated with a request from MH providers and researchers in Malawi who have long recognized the challenges faced by those working in under-resourced facilities..."
In conclusion: "Understanding factors that influence provider behavior (normative, structural, and behavioral) and developing pragmatic approaches to alleviate some of them may lead to improved quality of care, including more RMC. A multipronged approach is required, including empowering MH providers to deal with difficult situations and providing opportunities, such as providing group and individual counseling services, to help them overcome experiences related to high workload, trauma, or critical incidents....To be effective, interventions that are designed to promote MH provider behavior change must encourage an understanding of any entrenched attitudes, what motivates providers, values, and other more normative factors that drive how providers interact with clients, colleagues, and managers within the health system."
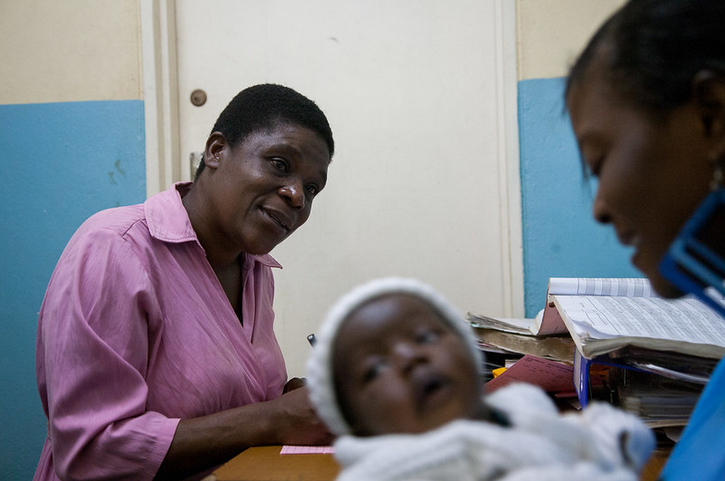
Global Health: Science and Practice August 2023, https://doi.org/10.9745/GHSP-D-23-00008. Image credit: Baylor College of Medicine Children's Foundation-Malawi / Robbie Flick via Flickr (CC BY-NC-ND 2.0)
- Log in to post comments












































