Coverage and Determinants of Influenza Vaccine among Pregnant Women: A Cross-sectional Study
National University of Singapore and National University Health System (Offeddu, Tam); London School of Hygiene & Tropical Medicine (Tam); Singapore General Hospital (Yong, L.K. Tan); KK Women's and Children's Hospital (Thoon, Lee, T.C. Tan, Yeo, Yung); Lee Kong Chian School of Medicine, NTU Imperial College (Yung)
The World Health Organization (WHO) recommends influenza vaccination for pregnant women. However, achieving high influenza vaccine coverage among this high-risk population remains challenging. This cross-sectional survey aimed to (i) determine the level of influenza vaccine coverage among pregnant women in Singapore, (ii) investigate pregnant women's knowledge, attitudes, and practices towards influenza vaccination in the local context, and (iii) identify factors associated with influenza vaccine uptake in this population.
Between September and November 2017, the researchers recruited pregnant women aged 21 years and older at two public hospitals in Singapore. Five hundred women completed an anonymous, self-administered online questionnaire based on the Health Belief Model of health behaviour. The questionnaire included domains assessing participants' demographics, vaccination history, knowledge, attitudes, insurance status, willingness to pay, cues to vaccination, and willingness to vaccinate.
Selected findings:
- The majority of participants (77%) were aware that there is an influenza vaccine. However, only 46% knew that influenza vaccination is recommended during pregnancy. A few misconceptions were identified among participants, such as the belief that influenza can be treated with antibiotics.
- 17% had received information about the influenza vaccine during their current pregnancy. The most common sources of information were friends, family, or employers (37%), although women most commonly indicated their obstetrician (71%) and official websites (40%), such as the Ministry of Health or Health Promotion Board websites, as their preferred sources of information.
- Only 49 women (9.8, 95% confidence interval (CI): 7.3-12.7%) reported receiving the vaccine during their current pregnancy. The most common reasons to get vaccinated against influenza during pregnancy were recommendation by a healthcare worker (57%) and protection from influenza in general (41%).
- Women who were personally advised to get vaccinated against influenza during pregnancy were 7 times more likely to be vaccinated (prevalence ratio (PR)=7.11; 95% CI: 3.92-12.90). However, only 12% of women were personally advised to get vaccinated. Of these, 34% were recommended by their obstetrician, while others were advised by their general practitioner (22%), a nurse (22%), or friends and family (21%).
- Other factors associated with vaccine uptake were vaccination during a previous pregnancy (PR=2.51; 95% CI: 1.54-4.11), having insurance to cover the cost of the vaccine (PR=2.32; 95% CI: 1.43-3.76), and higher vaccine confidence (PR=1.62; 95% CI: 1.30-2.01).
- Nearly half of unvaccinated women (48%) stated they were unlikely or very unlikely to get vaccinated during current gestation. The main reasons not to get vaccinated included lack of recommendation (45%) and lack of information on the influenza vaccine (31%).
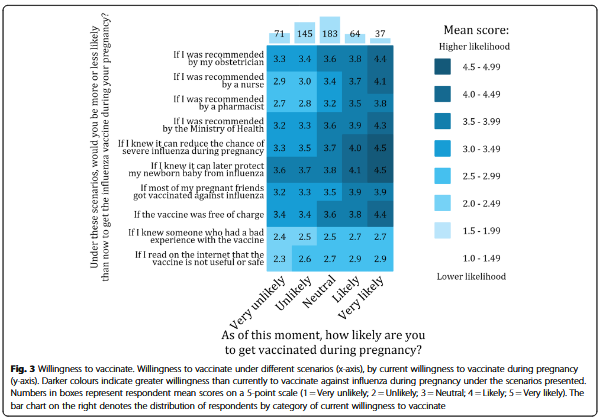
- A fraction of participants (14%) stated their willingness to vaccinate would not increase under any of the hypothetical scenarios presented. However, more than 60% stated that their willingness to vaccinate would increase if they knew that vaccination during pregnancy can protect them or their newborn from severe influenza illness. Other factors increasing participants' willingness to vaccinate included recommendations from an obstetrician or the Ministry of Health, and free vaccination.
The researchers cite other studies finding that healthcare providers who are more knowledgeable and confident about the influenza vaccine are more likely to recommend vaccination and obtain high coverage among expecting mothers. In Singapore, qualitative studies have revealed limited influenza vaccine acceptance among healthcare professionals. Thus, provider-targeted interventions involving education, automatic reminders, and vaccination training, which have been found to increase vaccination uptake among pregnant patients in other settings, may be worth exploring in Singapore. In contrast to other settings, this study indicates that the potential impact of pharmacy-led maternal influenza vaccination strategies may be limited in Singapore.
In conclusion: "Influenza vaccination uptake among pregnant women in Singapore is low. There is considerable scope for improving vaccination coverage in this high-risk population through vaccination recommendations from healthcare professionals, and public communication targeting common misconceptions about influenza and influenza vaccines."
BMC Public Health, volume 19, number 890 (2019). https://doi.org/10.1186/s12889-019-7172-8.
- Log in to post comments












































