Key Considerations for Successful Implementation of Maternal Immunization Programs in Low and Middle Income Countries
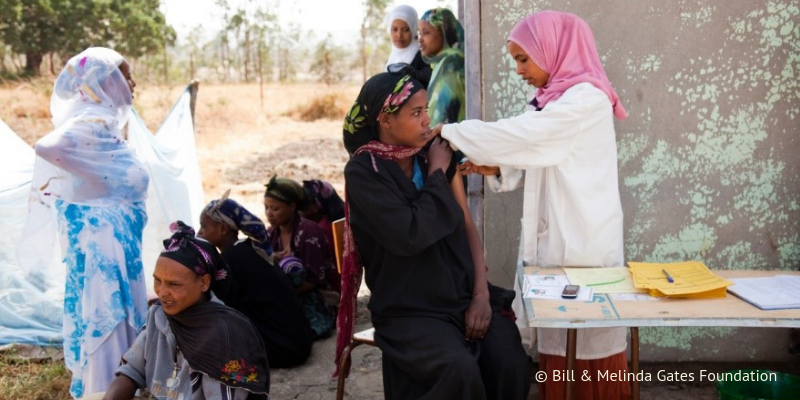
Monash University (Krishnaswamy, Giles); World Health Organization, or WHO (Lambach)
"The Maternal and Neonatal Tetanus Elimination Program serves as proof of concept that with adequate political will and resources, significant reduction in maternal and neonatal mortality can be achieved globally."
Maternal immunisation is a potentially promising strategy to reduce infection in neonates and infants, particularly in low- and middle-income countries (LMICs), where the burden of vaccine-preventable diseases (VPDs) is the greatest. Every 5 years, Gavi takes stock of available and expected vaccines to develop a new vaccine investment strategy and to set new priorities for its vaccine support programme through in-depth analysis and consultations. In an effort to close the gaps in knowledge required to inform policy, this review outlines 5 key elements for successful implementation of a maternal immunisation programme, focusing particularly on LMICs. This summary focuses on the communication-centred aspects.
The 5 elements, with associated challenges and recommendations, include:
- Knowledge of the local epidemiology and burden of disease: These data are often not available in resource-constrained settings, and these countries often have to revert to other information sources - for example, from countries with a similar epidemiology. "Given resource limitations, the availability, effectiveness, cost, and feasibility of alternative strategies for disease prevention should be considered to determine if maternal immunisation is in fact the most cost-effective approach."
- Involvement of pregnant women: Efforts beyond having national recommendations and evidence of vaccine efficacy and safety are often needed to convince pregnant women of the benefit and safety of maternal vaccination. To ensure uptake, women need to be made aware of potential benefits for the mother and the child. Healthcare providers play a central role in countering pregnant women's concerns by providing information and recommending vaccination. "Studies have demonstrated that women place most trust in their maternity care providers and so receiving education directly from their providers is likely to be the most effective strategy....As with any intervention during pregnancy, engagement and education of pregnant women is key to the successful implementation of the intervention. Understanding the multifactorial and complex causes of vaccine hesitancy in different contexts is important to be able to consider approaches at individual, provider, health system and national levels."
- Healthcare provider recommendation: As reported here, it is important to understand the awareness, attitudes, and perceptions of healthcare providers and the barriers to healthcare provider recommendation in the local context. One of the barriers is concern about vaccine safety. The WHO manual on implementing maternal influenza vaccination advises that "health worker training and overall communications on maternal influenza vaccination must carefully address safety issues and efficacy information." It is suggested that educational material be incorporated within resources that are accessible to maternity care providers and within existing training infrastructure. In addition, endorsement of maternal immunisation by the relevant health authorities can give healthcare providers confidence to recommend vaccines. Steps to embed vaccination within workplace culture, such as through reminders incorporated into antenatal records, can assist providers in viewing maternal vaccination as part of routine pregnancy care and as every provider's responsibility.
- Equitable access to maternal vaccination: "Vaccine supply and integration of immunization into antenatal care services are both important considerations for the success of maternal immunization programs. The structures that have ensured the success of maternal tetanus elimination programs may provide a platform on which to build future maternal vaccination programs."
- Systems for disease surveillance, programme evaluation, and safety monitoring: Among the suggestions: "To increase reporting and raise awareness of the importance of safety monitoring, training and education of healthcare workers and the community in detection and reporting of AEFIs [adverse events following immunisation], and strengthening of and linkage of health information systems and pregnancy registries are needed."
In conclusion: "To ensure optimal allocation of limited resources, LMICs in particular, will need to prioritize new vaccination programs targeting pregnant women based on the impact they could have on local burden of disease, and implementation-related aspects such as vaccine acceptability, vaccine safety and cost-effectiveness." The authors point to global efforts such as Advancing Maternal Immunization (AMI) and WHO's Maternal Immunization and Antenatal Care Situation Analysis (MIACSA), which aim to identify strategies and tools for decision-makers and implementers working on the introduction of new maternal vaccines.
Human Vaccines & Immunotherapeutics 2019, Vol. 15, No. 4, 942-50. https://doi.org/10.1080/21645515.2018.1564433. Image credit: © Bill & Melinda Gates Foundation
- Log in to post comments












































