Rethinking Strategies to Address Inequity in Immunization Services towards Achieving Universal Immunization Coverage (UIC) in Karachi, Pakistan
John Snow International, or JSI (Hossain, Masood, Shimp); Expanded Programme on Immunization (EPI), Pakistan (Sultan, Safdar, Younus); Gavi (Setayesh)
"...an example of a collaborative and participatory multi-step process between a variety of stakeholders to align support, decrease inequities and overcome implementation barriers of immunization services."
Due to the presence of a large number of unimmunised and under-immunised children in Karachi, this Pakistani city experiences frequent outbreaks of measles, and wild poliovirus (WPV) continues to circulate there. Reasons for low immunisation coverage include lack of demand and trust among people for immunisation services and lack of governance and accountability in a fragmented health management structure, among others. Nearly half (7 million, 45.5%) of Karachi's population resides in 988 slum areas, and people living in these unauthorised urban settlement areas are excluded from immunisation services. This paper highlights the process the Sindh Government, in collaboration with partners, undertook to address inequity in urban immunisation services in Karachi.
The strategy was developed through was a stepwise process, with multiple layers of stakeholders' input and feedback informing co-creation of evidence-based interventions:
- Situational analysis: From December 2018 to February 2019, the Expanded Programme on Immunization (EPI) reviewed existing literatures and conducted quantitative and qualitative data collection to identify gaps, barriers, and challenges of routine immunisation services in Karachi. For example, in addition to a household survey, visualisation through geographic information system (GIS) technology of existing immunisation service outlets and placement of vaccinators revealed patterns of inequity that may have been more difficult to identify if the data were presented in a tabular way. An example of the qualitative research was the holding of 27 focus group discussions with caregivers of zero-dose and partially immunised children to understand their barriers to accessing immunisation services. The FGDs revealed widespread fears and mistrust among people about immunisation, with a range of reasons including low quality of services, lack of information, fear of side effects, rumours, and lack of motivation.
- Two-day workshop for the stakeholders to develop strategy: A diverse group of stakeholders met in April 2019 to co-create strategies based on the findings of the situation analysis. Three technical working groups (TWGs) were formed to develop interventions in each of the three strategic areas: strengthening governance, leadership, and accountability; strengthening delivery of immunisation services in all areas; and increasing trust of and demand for immunisation services among people. Examples of interventions in the latter category included:
- Hiring communication officers at provincial and district level to develop and disseminate communication messages and materials;
- Conducting special communication activities in high-risk areas with messages in appropriate languages and means of communication;
- Involving local community leaders, indigenous leaders, and religious leaders for social mobilisation and message dissemination on immunisation; and
- Training health workers on interpersonal communication.
- Feedback from the District Health Team (DHT): The proposed strategies from all three TWGs were shared in June 2019 with DHTs in two districts (Central and East) for their feedback, and their input was incorporated into the interventions.
- Customisation of interventions for super-high-risk union councils (SHRUCs): The interventions were customised further in workshops in September-October 2019 for eight SHRUCs identified based on number of zero-dose children, presence of large slums, measles outbreaks, and ongoing circulation of WPV. Tailored action plans were developed for reaching zero-dose and under-immunised children and reducing dropout rates and missed opportunities of vaccination.
- Costing for the activities through a series of meetings in November 2019 with representatives from federal and provincial EPI and key partners, including aligning available domestic and donor funding for three years (2020-2022).
Reflecting on the interventions developed through this process, the paper's authors note that urban populations are more complex and socially heterogeneous than rural populations, comprising different ethnicities, social structures, cultural beliefs, and lack of community cohesion or resilience. Thus, health messages do not spread in urban areas as easily as in the rural areas. Thus, efforts to build community trust and demand for the services involved strategies such as engaging local traditional and religious leaders as messengers. In addition, alternative immunisation service delivery provisions (evening and/or weekend immunisation sessions) were included for children of working parents who are not able to utilise services during the regular sessions hours. In Bangladesh, such communication initiatives and extended hours of immunisation services were found to have significantly improved full immunisation coverage rates among children of working parents in slum areas.
In conclusion: "The scale-up of the similar initiative to different cities throughout Pakistan, and replicating the process for achieving universal health coverage (UHC) will rely on the flexibility of the strategy and the commitment from stakeholders' for engagement in the planning, implementation and monitoring processes."
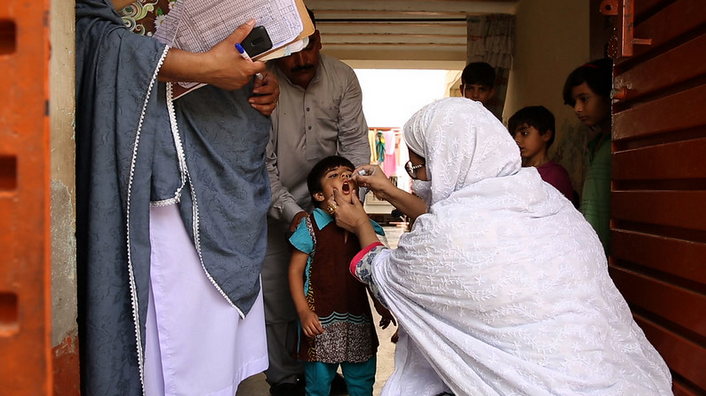
World Journal of Vaccines, 11, 39-49. https://doi.org/10.4236/wjv.2021.114006. Image credit: Sanofi Pasteur / Almeena Ahmed / Sanaullah Afridi via Flick ((CC BY-NC-ND 2.0)
- Log in to post comments












































